On a recent field trip to Tasmania, where I had managed to imbed myself with the Australian Digital Health Agency (ADHA), I found myself stuck in in the back seat of a smallish SUV, pinned between two senior ADHA minders.
Following a particularly robust public forum in the morning we, somewhat oddly, appeared to be heading out of town south of Hobart.
“Where to next,” I enquired of my chaperones. “Australian Antarctic Division”, came the reply.
Antarctica? My brain tried to make the connection but no obvious links came to mind. I figured we might be on a break. After all, who doesn’t like penguins and lots of snow?
Our host at the Australian Antarctic Division was Dr Jeff Ayton, Chief Medical Officer of the Polar Medicine Unit.
Dr Ayton, a previous president of the Australian College of Rural and Remote Medicine, and a well-known extreme-medicine expert, opened with a story that made it immediately clear why we’d been brought here.
Doctors who practice in Antarctica are arguably the most extreme practitioners of generalised medicine in the world.
They are GPs who do much of their more difficult work via relatively tenuous communication links to the mainland. They don’t have the luxury of a nearby hospital or pathology lab if things get hairy, or an easy call to a local specialist if something is particularly strange and potentially awkward.
In order to improve their chances of saving lives and managing complex cases, everything has, over many years of operation and planning, been optimised to extreme levels in this unit. This means telehealth systems, the storage and analysis of electronic health records, secure messaging, expert-decision support, medical wikis, patient-management software, communication protocols and so on.
This unit turns out to be a potential microcosm of the future of a national Australian “connected” healthcare system and, in some ways, the future of the “general” practice of medicine.
It’s sort of an accident that it exists. It’s been created by the necessity to have the most perfectly connected and serviced general practice in the world — because it’s in Antarctica.
The insights that this unit provides into what is actually feasible, using the latest in innovative technology, clever co-ordination, and co-operation between normally disparate medical groups, are nothing short of amazing.
One GP (over winter), well resourced, connected to decent expert systems and with the right protocols and links to support services, can do a heck of a lot by themselves. Well, by themselves, but with very well-engineered telehealth support from experts when things go belly up.
Although it’s clearly challenging work, it’s also highly rewarding and wildly efficient. If any of this is in the future of being a GP, then there is cause for quite a bit of optimism for the profession.
As Dr Ayton casually ran us over the basics, it felt like I was watching Towards 2000 when I was a kid. Nearly all of what he described I’d only heard about in plans and discussions from the likes of medical software entrepreneurs and senior visionary health bureaucrats.
But Dr Ayton has this all working today in his unit. Ayton and his technical crew have spent years quietly and diligently honing and refining the systems to make our Antarctic stations work medically at an incredibly efficient level. And connected technology is a big part of what they’ve managed to crack.
The unit started a fully networked electronic health record system in 2009 and they started collecting electronic health records as early as 1989. It’s comprehensive. Although not actually cloud-based (that’s too difficult with the data communication issues), it’s seamless between the various Australian Antarctic stations and the mainland. It can talk to the My Health Record, directly to pathology labs and to various other important ancillary services.
The records are precise and longitudinal over many years and, as a result, the data is starting to provide the unit with valuable insights into the preparation, servicing and delivery of healthcare on the stations.
Each station staff member has full access to a full and well-organised electronic medical record via a web connection with all the associated privacy settings and permissions.
Today, thankfully, Antarctic Division Polar Medicine doctors use satellite links. But this is still tricky. Delays in audio of several seconds can occur. And if you’re sending data back and forth, as you do when having to get a second opinion on a scan or X-ray, or the like, the maximum bandwidth speed is something akin to an AOL internet connection in the early 1990s. At 356 bps, it’s nearly that slow.
Notwithstanding, the unit has managed to achieve some telehealth support for the stations which is highly efficient, and something which most GP practice owners would love to have as a part of their services.
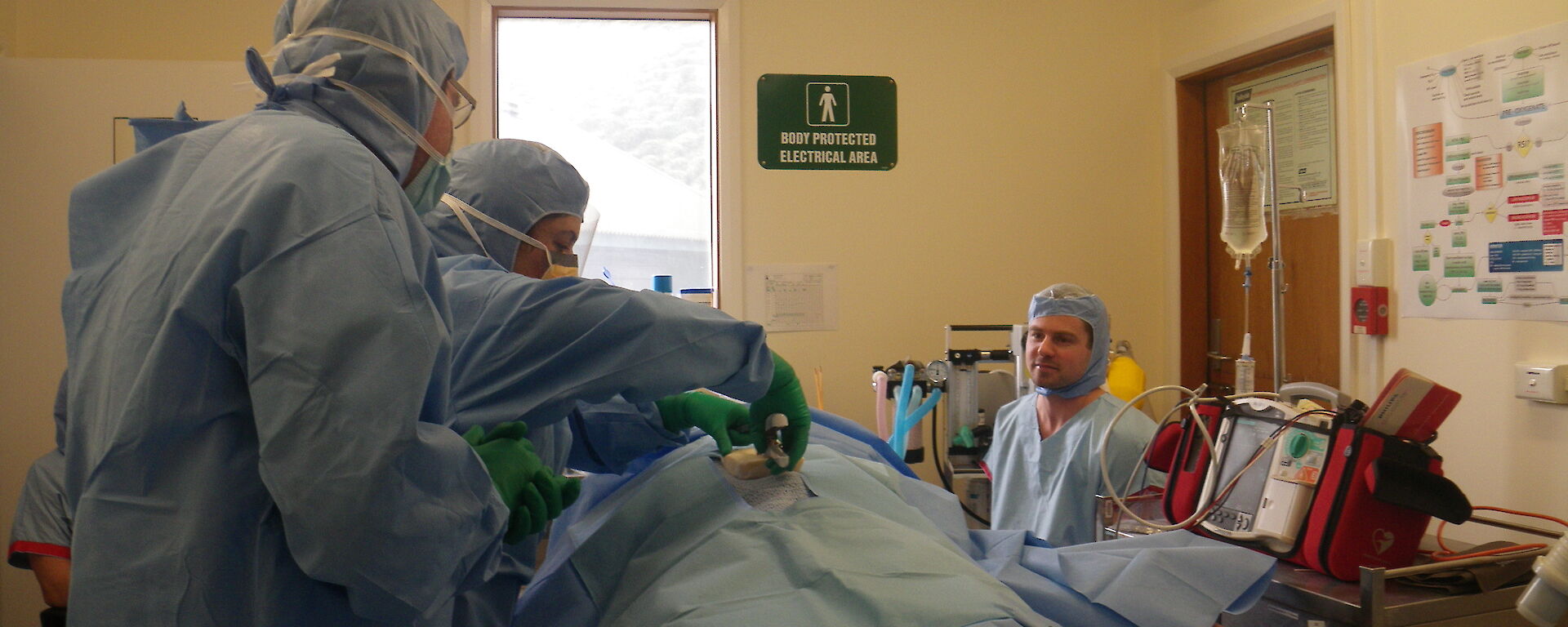
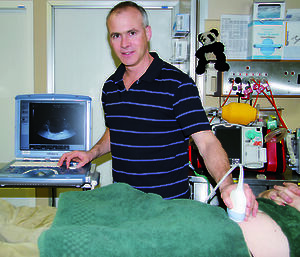
When something really goes wrong, the surgery on the station in Antarctica goes online to the Division’s headquarters back at Hobart, where the Antarctic doctors have tele-access to a range of sophisticated gear. This includes blood chemistry analysis, X-ray, ultrasound, and more.
The unit is currently looking at using robotic surgery remotely, where a trained surgeon on the mainland can perform the operation via telehealth. Currently, when things get this complex, the GP is being guided to do their work via audio from a surgeon in Hobart.
If that all sounds a bit scary, then spare a thought for the doctor on call at Casey station in the winter of 1961, when one of the station staff suffered a brain aneurysm.
To prepare for this surgery, which ended up saving the station member’s life, the assistants on the mainland had to communicate multiple times via telex, including getting the station’s plumber to make the various instruments that were required for the operation.
Recently, with the only doctor on one of the stations injured in a fall, and with tele-surgery support, a non-doctor was able to perform complex surgical procedures on the injured doctor, allowing that doctor to recover and resume duties at the station.
Other alarming Antarctic surgical stories include that of a Russian doctor who, facing acute appendicitis on the Russian Antarctic station in 1961, and with no-one capable of helping, operated on himself. During the operation he lost consciousness, but later awoke to complete the procedure and make a full recovery.
Not to be outdone by the Russians, Dr Jerri Lin Nielsen, an American doctor with a background in emergency medicine, famously self-treated her breast cancer while working at the Amundsen-Scott South Pole station in 1998.
There has been a doctor on Australia’s Antarctic stations since the establishment of the first station there in 1947. Initial medical contact with the mainland for earlier expeditions was via morse code and later via HF radio, both of which were relayed via Macquarie Island and both of which were notoriously unreliable. A full medical unit was established in Australia to support the Australian Antarctic stations in 1963. At that time communication was via telex machine.
What the Polar Medicine Unit of the Australian Antarctic Division confirms for us is that everything that technology promises, is actually possible. It does work, it does create enormous efficiency, it can make a GP’s job more interesting and less isolated. And it’s not that expensive.
It’s a matter of organisation, co-ordination focus and co-operation. That, of course, is no small problem across the Australian healthcare system. But at least we know we can do this stuff if we really want to.
Jeremy Knibbs
The Medical Republic
This is an edited version of an article that first appeared in The Medical Republic on 9 February 2017.